Inappropriate concomitant medication prescribing remains one one of the major causes of protocol violations within clinical trials.
Investigator Analysis
CliniSafe undertook a survey of Investigators and revealed:
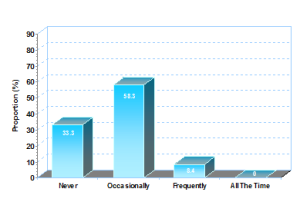
67% of CRAs confirmed that they have experienced patients enrolled in error into studies due to prohibited medications with occasional to frequent occurrence.
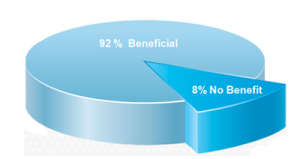
92% of Investigators felt a quick and effective system to monitor concomitant medications would be beneficial to their practice.
A variety of problems can occur when protocol exclusion information on concomitant medication use is distributed to medical professionals as paper documentation.
... lack of Width
Width is referred to by the WHO as the total number of medications within databases. Paper protocols are inherently faced with the difficulty in incorporating a list of all medications. Terminology such as “… and similar drugs.” is common and often unhelpful.... lack of Depth
Depth is referred to by the WHO as the information detail provided on each drug. Paper formularies are simply unable to provide this level of detail. The drugs listed in the protocol often only include the generic names of the drug.... use of Formularies
Drugs have to be looked up in printed formulary books. This is time consuming and error prone. It is therefore easy for a busy clinician to inadvertently overlook or prescribe an excluded medicine.
Implementing protocol concomitant medication changes for safety reasons may need to be done without delay. On other occasions it follows review amendment by appropriate authorities. In either case reliably disseminating these changes creates an error prone environment for all those working on the protocol. Electronic version control within CliniSafe provides a seamless way of implementing change.
Coding to Umbrella categories within clinical trials is often avoidable. Missing data in clinical trials can seriously undermine analysis.
Tools that improve site efficacy and improve investigator performance inevitably help your study. The commonest delay in clinical trials results from slow patient enrolment.
Concomitant medications are usually restricted because they either effect the data or the subjects safety. There are numerous examples where patients in studies on excluded medications have effected data and caused failed studies. Reducing potential inadvertent effects on participants health is a key goal for all working within clinical trials and although mortality from concomitant medication prescribing errors is fortunately uncommon it is not unknown.